Mammography: Does Breast Cancer Early Detection Save Lives?

This article on early detection for breast cancer with mammography is a chapter from my book Cancer Cured. If you find it helpful, please support my work and buy my book on Amazon.
LIKE ALL BUSINESSES, the cancer industry requires a steady flow of customers in order to generate revenue. The way it accomplishes this is by popularizing the idea that detecting and treating cancer in its early stages improves survival. ‘Early detection saves lives’ is a marketing strategy used to motivate people who have no signs or symptoms of cancer, to undergo regular screening for cancer.
The World Health Organization claims that “Cancer mortality can be reduced if cases are detected and treated early,”1 and the American Cancer Society states, “Most doctors feel that early detection tests for breast cancer save thousands of lives each year. Many more lives probably could be saved if even more women and their health care providers took advantage of these tests.”2
Let’s investigate the evidence for and against mammography so you can decide for yourself if you think early detection saves lives.
TABLE OF CONTENTS
Mammography – Breast Cancer Screening
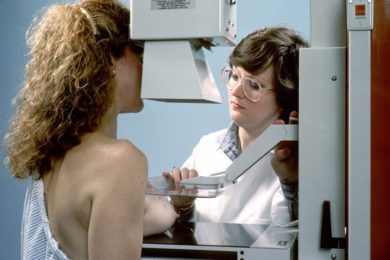 First introduced in the 1970’s,26 mammography is an x-ray procedure that captures a photograph of the human breast used to detect breast cancer. While those who are invested in expensive mammography machinery or who rely on breast cancer screening to earn a living will assure you that mammography reduces breast cancer death rates, a number of large-scale studies have demonstrated that mammography provides no mortality benefit.27-29
First introduced in the 1970’s,26 mammography is an x-ray procedure that captures a photograph of the human breast used to detect breast cancer. While those who are invested in expensive mammography machinery or who rely on breast cancer screening to earn a living will assure you that mammography reduces breast cancer death rates, a number of large-scale studies have demonstrated that mammography provides no mortality benefit.27-29
A Closer Look…
- The Canadian National Breast Screening Study 1 involved 50,000 women aged 40 to 49 years and compared women who received 5 years of annual mammography screening and physical breast examinations with women who received only one physical breast examination. The study found that five annual mammograms and breast examinations in women aged 40 to 49 caused “no reduction in breast cancer mortality.”27
- The Canadian National Breast Screening Study 2 involved 40,000 women aged 50 to 59 years and compared women who received five years of physical breast exams and mammography screening with women who received physical examinations only. The study concluded that in women aged 50 to 59, “the addition of annual mammography screening to physical examination has no impact on breast cancer mortality.”28
- The 25-year combined follow-up of the Canadian National Breast Screening Study 1 and 2 was one of the largest and most meticulous studies ever conducted on mammography. Published in the British Medical Journal in 2014, results showed that “Annual mammography in women aged 40-59 does not reduce mortality from breast cancer beyond that of physical examination…”29
Overdiagnosis and Overtreatment
One of the major failures of mammography is how frequently it results in misdiagnosis of breast cancer. Over the course of 10 mammograms, women in the United States have between a 58-77% chance of being falsely diagnosed with breast cancer.30 Another study found that for women with multiple breast cancer risk factors, like a strong family history, prolonged use of the contraceptive pill, etc. – the ones most strongly urged to have annual mammograms – the 10-year cumulative risk of being falsely diagnosed is “as high as 100 percent.”31 And of course, most will end up undergoing unnecessary treatments and suffering the horrendous side effects and mutilations associated with surgery and radiotherapy.
A 2012 study published in the New England Journal of Medicine concluded that one in three women (33%) diagnosed with breast cancer from a mammogram are misdiagnosed, and that a whopping 1.3 million women have been overdiagnosed by mammography in the past 30 years.32
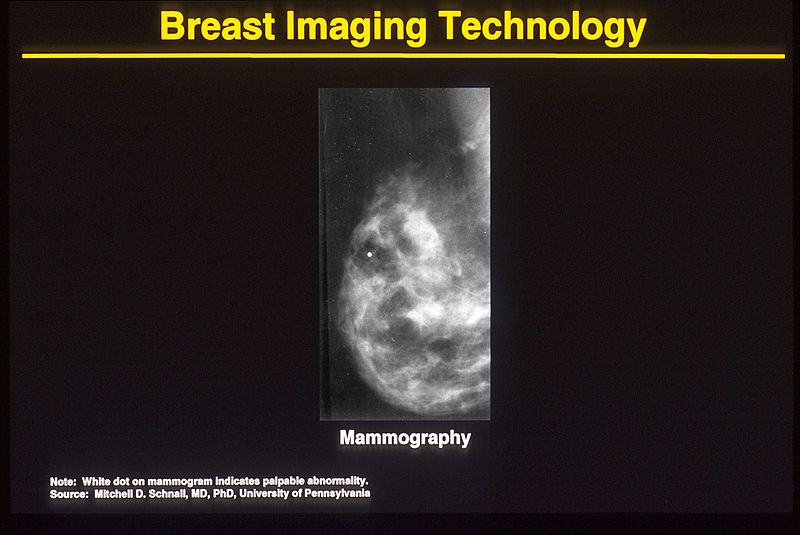
A BIG Price to Pay
Although the PSA test and mammography both fail to achieve their intended purpose of prolonging life, the PSA test involves only a blood sample while mammography exposes patients to damaging ionizing radiation and other harmful procedures.
First, the breast is tightly (and often painfully33) compressed between two imaging plates. If cancer is present in the breast during this compression it can result in metastasis.34 Next, the x-ray image is taken and the patient receives a 10 mSv (millisievert) dose of ionizing radiation, approximately “1000 times greater than that from a chest x-ray,” according to Dr. Samuel Epstein.35
The Dangers of Low-Dose Ionizing Radiation
The US government has long-held the position that low-doses of ionizing radiation are not hazardous to human health,36 but since the early 1950’s scientific research has indicated repeatedly that low-doses of radiation, like those administered to patients during x-ray imaging, do in fact cause increased rates of cancer.37-53
A Closer Look…
- Researchers from the University of California investigated the relationship between x-ray exposure early in life and childhood leukemia in 2010. “Exposure to post-natal diagnostic X-rays is associated with increased risk of childhood ALL [acute childhood leukemia], the study concluded.”53
- A 1981 study published in The Lancet looked at cancer incidence in female factory workers who had been producing paint containing the radioactive element radium. The workers received radiation doses of 1-4mGy (milligray) per week and the study found, “Those in the group who were under 30 years of age when they started work show a significantly increased risk of dying from breast cancer.”46
- In 1989, scientists from Atlanta, Georgia investigated 1,030 women with scoliosis who had received multiple x-rays during childhood. Published in The Journal of the National Cancer Institute, at an average follow-up of 26 years, the study found an 83% greater incidence of cancer in the women compared to the general population. Importantly, their rate of cancer actually increased with time; women assessed more than 30 years later had a 140% greater incidence of cancer than the general population.43
Low Doses Worse Than Higher Doses
Groundbreaking research, mostly on atomic bomb survivors and nuclear workers, is beginning to uncover a startling detail – not only are low doses of ionizing radiation enough to cause cancer, but low doses can actually be more harmful than larger ones.54-57 E.B. Burlakova, director of the Radiobiology Committee of the Russian Academy of Sciences, has published a number of studies showing that the true dose-response of ionizing radiation is biphasic, meaning the damage increases from zero dose and then falls and then increases again.58
A Closer Look…
- A 2008 study from Japan compared cancer prevalence in Hiroshima atomic bomb survivors with an unexposed population. The study found a significantly elevated risk of cancer in the exposed population, “Even at low and very low dose categories.”56
- Italian researchers exposed a group of mice to 1 Gy (gray) of ionizing radiation and another group of mice to 0.1 Gy of ionizing radiation and compared the effects. Results were published in the International Journal of Radiation Biology in 2008 and found, “In mice exposed to 1 Gy genetic damage was initially high and decreased during the experimental-time, while in the 0.1 Gy group damage, a first low, persisted and slightly increased.”54
- In 2016, researchers from Germany and Latvia questioned the validity of the current worldwide radiation risk model by investigating the genetic risks of exposure to low doses of radiation. The study found that, “Nearly all types of hereditary defects were found at doses as low as one to 10 mSv” and concluded that the current worldwide risk model for genetic effects of ionizing radiation is unsafe. Importantly, their work “supports a dose response relationship which is non-linear and is either biphasic or supralinear (hogs-back) and largely either saturates or falls above 10 mSv.”57
How can a lower dose of ionizing radiation be more harmful than a larger dose?
“Cancer arises when the DNA in cells is damaged, but the cells are not killed. Higher radiation doses are more likely to kill cells outright. So the lower doses are disproportionately carcinogenic,” explains scientist Dr. Chris Busby.59
I asked Dr. Ray Peat the same question and he wrote, “The greatest effect per dose at low doses is sort of analogous to a car getting good gas mileage at low speeds with low wind resistance, compared to poor gas mileage at 80 to 100 mph, with considerable wind resistance. It isn’t surprising if you think in terms of ‘relatively mild electronic excitation,’ producing chronic inflammatory signals, rather than all-or-nothing mutagenic events.”
Is X-Ray Imaging Worth The Risk?
A number of outspoken scientists have come to some startling conclusions regarding the use of medical imaging that the world needs to know about.
In 1971, Dr. Robert W. Gibson and his colleagues at the University of Buffalo conducted a study on the health effects of low-dose radiation from x-ray imaging. The researchers concluded that undergoing less than a dozen routine medical x-rays to the same part of the body increases the risk of leukemia by at least 60%.60
Dr. Irwin Bross headed the Tri-State Leukemia Study in the 1970’s to determine what had been causing the alarming increases in leukemia at the time. The experiment included 16 million people from New York, Maryland, and Minnesota, and after exploring wide-ranging factors – including health history, occupational history, residential history, family background, cause of death for parents and grandparents, exposure to farm animals, pet ownership, whether or not the pets had ever been sick – Dr. Bross concluded that medical radiation in the form of diagnostic medical x-rays was the main cause of the rising rates of leukemia.61
Dr. John Gofman, medical physicist from the University of California, became a spokesman for the United States Atomic Energy Commission in the 1940’s and spent almost 30 years travelling around glorifying the use of x-rays and other forms of radiation while denying that ionizing radiation had any harmful effects. Then, right in the middle of one of his speeches in the late 1960’s, he realized that what he had been saying for three decades was insane:
“The big moment in my life happened while I was giving a health lecture to nuclear engineers. In the middle of my talk it hit me! What the hell am I saying? If you don’t know whether low doses are safe or not, going ahead is exactly wrong. At that moment, I changed my position entirely.”
Dr. Gofman suddenly went from being a government and nuclear industry ‘talking head’ to one of their biggest threats and found himself campaigning against the use of nuclear and medical x-ray technologies as well as writing a number of groundbreaking books.
The most significant conclusion made by Dr. Gofman after a lifetime of investigation into the biological effects of low-dose x-ray radiation was that accumulated radiation exposure from medical diagnostics is the main cause of over 50% of cancer deaths, 60% of heart disease deaths and over 80% of breast cancer deaths in the United States. While Dr. Gofman acknowledged other causes of cancer such as smoking, poor food quality and environmental toxins, he maintained that more than half the deaths from cancer and heart disease would not have occurred if it weren’t for medical x-rays.62
Of course, none of the evidence above can be officially acknowledged or it would mean the death of the entire nuclear industry: power, weapons and medical imaging.
Cancer Screening: A public health disaster
If mammography reveals an abnormality that the doctor suspects might be cancer, a biopsy will be performed. And if the biopsy reveals what the doctor interprets to be cancer, the woman suddenly becomes a breast cancer patient and will receive the whole works – surgery, chemotherapy and radiotherapy.
Despite evidence showing that surgical removal of one or both breasts (mastectomy) results in increased tumor recurrences and higher mortality,63 or at best provides no additional benefit,64 mastectomies have been on the rise in recent years.65
A Closer Look…
- A 1995 study published in the New England Journal of Medicine followed up with breast cancer patients 10-years after receiving a mastectomy (surgical removal of one or both breasts) or a simple lumpectomy (surgical removal of only the tumor and some surrounding tissue) followed by whole-breast irradiation. Patients who received the mastectomy had more tumor recurrences and higher mortality 10-years following treatment than those who received the less invasive lumpectomy.63
This trend has a lot to do with the dramatic increase in biased media coverage of celebrity mastectomies since 2004, wrote scientists from the University of Michigan. “The surgical treatment was significantly more likely to be mentioned [in the media] when a celebrity had bilateral mastectomies than unilateral mastectomy or breast conservation,” their study concluded.66
One of the side effects a surgeon will probably fail to mention before performing a mastectomy is the subsequent almost-universal decline in self-esteem that women experience following the procedure.67,68 “Patients who had had a mastectomy felt less attractive, less sexually desirable, and more ashamed of their breasts. They also experienced less enjoyment in their sexual relationships than they had before treatment.”69 To combat this hopelessness, many women return to their surgeons for breast implants, which unfortunately, only make a bad situation worse; as breast implants following mastectomy have been associated with a 3-fold increase in the risk of suicide.70
Now we return to our original question from the beginning of this chapter: Does early detection and treatment of cancer save lives?
We’ve examined a number of studies showing that neither the PSA test nor mammography provide any mortality benefit whatsoever to the men and women who undergo them. Rather than saving lives, the widespread implementation of prostate and breast cancer screening has only enhanced the amount of men and women diagnosed and treated for cancer.
While this is obviously a lucrative and rewarding situation for the cancer industry, the mass overdiagnosis and overtreatment that sustains the booming cancer business comes at a considerable price; it means patients are frequently told they have cancer when they don’t, and are frequently treated aggressively for diseases they don’t have.
Maybe this is why Dr. Dean Burk once said of the American Cancer Society, “They lie like scoundrels,” or why Dr. James Watson, the man who discovered DNA, declared before the California Assembly Committee of Health in 1976, “The American public is being sold a nasty bill of goods about cancer… Today, the press releases coming out of the National Cancer Institute have all the honesty of the Pentagon’s.”
References
1. World Health Organization. (2017). Cancer Fact Sheet. Available: http://www.who.int/mediacentre/factsheets/fs297/en. [February 3rd, 2017].
2. American Cancer Society. Breast Cancer Early Detection and Diagnosis. Available: https://www.cancer.org/cancer/breast-cancer/screening-tests-and-early-detection.html. [January 15th, 2017].
26. Retsky M, Demicheli R, Hrushesky W, Baum M, Gukas I. Surgery triggers outgrowth of latent distant disease in breast cancer: an inconvenient truth?. Cancers (Basel). 2010;2(2):305-37.
27. Miller AB, To T, Baines CJ, Wall C. The Canadian National Breast Screening Study-1: breast cancer mortality after 11 to 16 years of follow-up. A randomized screening trial of mammography in women age 40 to 49 years. Ann Intern Med. 2002;137(5 Part 1):305-12.
28. Miller AB, To T, Baines CJ, Wall C. Canadian National Breast Screening Study-2: 13-year results of a randomized trial in women aged 50-59 years. J Natl Cancer Inst. 2000;92(18):1490-9.
29. Miller AB, Wall C, Baines CJ, Sun P, To T, Narod SA. Twenty five year follow-up for breast cancer incidence and mortality of the Canadian National Breast Screening Study: randomised screening trial. BMJ. 2014;348:g366.
30. Von euler-chelpin M, Kuchiki M, Vejborg I. Increased risk of breast cancer in women with false-positive test: the role of misclassification. Cancer Epidemiol. 2014;38(5):619-22.
31. Christiansen CL, Wang F, Barton MB, et al. Predicting the cumulative risk of false-positive mammograms. J Natl Cancer Inst. 2000;92(20):1657-66.
32. Bleyer A, Welch HG. Effect of three decades of screening mammography on breast-cancer incidence. N Engl J Med. 2012;367(21):1998-2005.
33. Kornguth PJ, Keefe FJ, Conaway MR. Pain during mammography: characteristics and relationship to demographic and medical variables. Pain. 1996;66(2-3):187-94.
34. Van netten JP, Cann SA, Hall JG. Mammography controversies: time for informed consent?. J Natl Cancer Inst. 1997;89(15):1164-5.
39. 35. Epstein SE. 2002. Mammography Doesn’t Come Without Risk. Los Angeles Times. Available: http://articles.latimes.com/2002/feb/25/opinion/oe-epstein25 [February 3, 2017].
36. Sept 29, 2015. Pt. 1 – Medical X-rays and Breast Cancer – Dr. John Gofman. Available: https://www.youtube.com/watch?v=AzW0zIjKcmE [February 3, 2017].
37. Modan B, Ron E, Werner A. Thyroid cancer following scalp irradiation. Radiology. 1977;123(3):741-4.
38. Boice JD, Preston D, Davis FG, Monson RR. Frequent chest X-ray fluoroscopy and breast cancer incidence among tuberculosis patients in Massachusetts. Radiat Res. 1991;125(2):214-22.
39. Baverstock KF, Vennart J. A note on radium body content and breast cancer in U.K. radium luminisers. Health Phys. 1983;44 Suppl 1:575-7.
40. Boice JD, Monson RR. Breast cancer in women after repeated fluoroscopic examinations of the chest. J Natl Cancer Inst. 1977;59(3):823-32.
41. Boice JD, Rosenstein M, Trout ED. Estimation of breast doses and breast cancer risk associated with repeated fluoroscopic chest examinations of women with tuberculosis. Radiat Res. 1978;73(2):373-90.
42. Harvey EB, Boice JD, Honeyman M, Flannery JT. Prenatal x-ray exposure and childhood cancer in twins. N Engl J Med. 1985;312(9):541-5.
43. Hoffman DA, Lonstein JE, Morin MM, Visscher W, Harris BS, Boice JD. Breast cancer in women with scoliosis exposed to multiple diagnostic x rays. J Natl Cancer Inst. 1989;81(17):1307-12.
44. Miller AB, Howe GR, Sherman GJ, et al. Mortality from breast cancer after irradiation during fluoroscopic examinations in patients being treated for tuberculosis. N Engl J Med. 1989;321(19):1285-9.
45. Modan B, Chetrit A, Alfandary E, Katz L. Increased risk of breast cancer after low-dose irradiation. Lancet. 1989;1(8639):629-31.
46. Baverstock KF, Papworth D, Vennart J. Risks of radiation at low dose rates. Lancet. 1981;1(8217):430-3.
47. Myrden JA, Hiltz JE. Breast cancer following multiple fluoroscopies during artificial pneumothorax treatment of pulmonary tuberculosis. Can Med Assoc J. 1969;100(22):1032-4.
48. Giles D, Hewitt D, Stewart A, Webb J. Malignant disease in childhood and diagnostic irradiation in utero. Lancet. 1956;271(6940):447.
49. Stewart A, Webb J, Hewitt D. A survey of childhood malignancies. Br Med J. 1958;1(5086):1495-508.
50. Stewart A, Kneale GW. Radiation dose effects in relation to obstetric x-rays and childhood cancers. Lancet. 1970;1(7658):1185-8.
51. Andrieu N, Easton DF, Chang-claude J, et al. Effect of chest X-rays on the risk of breast cancer among BRCA1/2 mutation carriers in the international BRCA1/2 carrier cohort study: a report from the EMBRACE, GENEPSO, GEO-HEBON, and IBCCS Collaborators’ Group. J Clin Oncol. 2006;24(21):3361-6.
52. Giles D, Hewitt D, Stewart A, Webb J. Malignant disease in childhood and diagnostic irradiation in utero. Lancet. 1956;271(6940):447.
53. Bartley K, Metayer C, Selvin S, Ducore J, Buffler P. Diagnostic X-rays and risk of childhood leukaemia. Int J Epidemiol. 2010;39(6):1628-37.
54. Giovanetti A, Deshpande T, Basso E. Persistence of genetic damage in mice exposed to low dose of X rays. Int J 58. Radiat Biol. 2008;84(3):227-35.
55. Goto H, Watanabe T, Miyao M, Fukuda H, Sato Y, Oshida Y. Cancer mortality among atomic bomb survivors exposed as children. Environ Health Prev Med. 2012;17(3):228-34.
56. Watanabe T, Miyao M, Honda R, Yamada Y. Hiroshima survivors exposed to very low doses of A-bomb primary radiation showed a high risk for cancers. Environ Health Prev Med. 2008;13(5):264-70.
57. Schmitz-feuerhake I, Busby C, Pflugbeil S. Genetic radiation risks: a neglected topic in the low dose debate. Environ Health Toxicol. 2016;31:e2016001.
58. Burlakova, E.B. 2000. Low Doses of Radiation: Are They Dangerous? Nova Science Pub Inc. 378 pps.
59. Busby, C. (2016). The ‘Genetics’ letter, the Euratom suicide clause, and the death of the nuclear industry. The Ecologist. Available: http://www.theecologist.org/campaigning/2988466/the_genetics_letter_the_euratom_suicide_clause_and_the_death_of_the_nuclear_industry.html. [February 3, 2017].
60. W. Gibson, M.D., National Enquirer, December 5, 1971, 11) as reported in the book Indicted!: The People Vs the Medical & Drug Cartel by James Henderson. (2009).
61. Leslie Freeman, ed., Nuclear Witnesses: Insiders Speak Out, New York: Norton, 1982, p.27.
62. Peat, R. (2011). Radiation and growth: Incoherent imprinting from inappropriate irradiation. Available: http://raypeat.com/pdf/Radiation-and-Growth-January-2011.pdf. [February 3, 2017].
66. 63. Jacobson JA, Danforth DN, Cowan KH, et al. Ten-year results of a comparison of conservation with mastectomy in the treatment of stage I and II breast cancer. N Engl J Med. 1995;332(14):907-11.
64. Vila J, Gandini S, Gentilini O. Overall survival according to type of surgery in young (≤40 years) early breast cancer patients: A systematic meta-analysis comparing breast-conserving surgery versus mastectomy. Breast. 2015;24(3):175-81.
65. Kummerow KL, Du L, Penson DF, Shyr Y, Hooks MA. Nationwide trends in mastectomy for early-stage breast cancer. JAMA Surg. 2015;150(1):9-16.
69. 66. Sabel MS, Dal cin S. Trends in Media Reports of Celebrities’ Breast Cancer Treatment Decisions. Ann Surg Oncol. 2016;23(9):2795-801.
67. Polivy J. Psychological effects of mastectomy on a woman’s feminine self-concept. J Nerv Ment Dis. 1977;164(2):77-87.
68. José Manuel García Arroyo and María Luisa Domínguez López, “Psychological Problems Derived from Mastectomy: A Qualitative Study,” International Journal of Surgical Oncology, vol. 2011, Article ID 132461, 8 pages, 2011.
69. Margolis G, Goodman RL, Rubin A. Psychological effects of breast-conserving cancer treatment and mastectomy. Psychosomatics. 1990;31(1):33-9.
70. Le GM, O’malley CD, Glaser SL, et al. Breast implants following mastectomy in women with early-stage breast cancer: prevalence and impact on survival. Breast Cancer Res. 2005;7(2):184-193.
